-
Introduction To Hip Replacement Surgery
+Replacement surgery of the hip is being successfully performed for the last forty years every year thousands of patients benefit from this surgery hip replacement India.
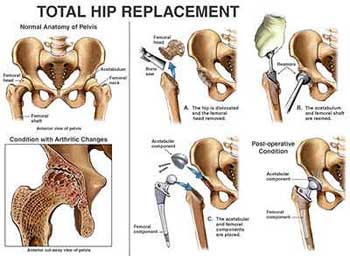
For variety of hip disorders, this operation helps in relieving pain, gaining range of motion and improving walking ability. It converts a disabled person to an able person. It converts a liability to an asset.
If you are advised hip replacement surgery, it is natural that you would want to know more about it. Here you will get all the information that you wish to know, in simple words, I have tried to explain what to expect before, during and after the surgery. It is meant to help you understand the intricacies of this complex surgery. In simple language, you are told, what will be done for you by the medical and paramedical staff and that you are required to do to achieve the desired result.
It is recommended that you go through information before you undergo the surgery. If you have any questions, our team of doctors will be happy to answer them.
The schedule given here is guideline, individual variations may occur. The result may vary in different individuals, and in two operated hips in the same individual.
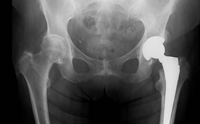 Knee replacement in India, the result depends on various factors like the cause of arthritis, age and general condition of the patient, condition of the joint, affection of other joints of the body.
Knee replacement in India, the result depends on various factors like the cause of arthritis, age and general condition of the patient, condition of the joint, affection of other joints of the body.No guarantee of any kind can be given for any surgical procedure. However, on an average the artificial joint works well up to 10 years in majority of cases. Further, with encouraging reports of success up to 20 years is also been seen.
Every surgery carries certain risks. You are required to make yourself familiar with these risks and the shortcomings.
-
First Consultancy
+When you come for the first consultation for hip pain to Dr. Rakesh Rajput, it is advisable to come with a prior appointment unless it is an emergency, so that when you come to the clinic your time is spent fruitfully.
Kindly expect to spend about one hour and 30 minutes for your first consultation. This time is spent in obtaining detailed history, performing thorough clinical examination, for taking x-rays and advising the treatment.
-
X-Rays
+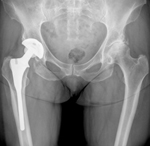 Treatment for hip disorders is advised taking into consideration your age, medical history, the intensity of pain, findings of clinical examination and x-rays.
Treatment for hip disorders is advised taking into consideration your age, medical history, the intensity of pain, findings of clinical examination and x-rays.Good quality x-rays in different positions are invaluable in arriving at correct diagnosis and for planning further management. Depending on the x-ray findings, the implant is selected.
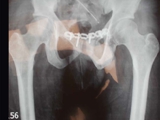
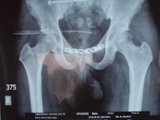
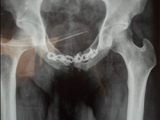
X-rays findings also decide the steps required to correct the deformity. Therefore, it is advisable to take x-rays under supervision of our staff for standardization.
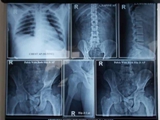
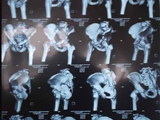
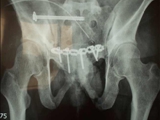
X-Rays of Pelvis
-
When you need Operation
+Conditons Requiring A Hip Replacement:
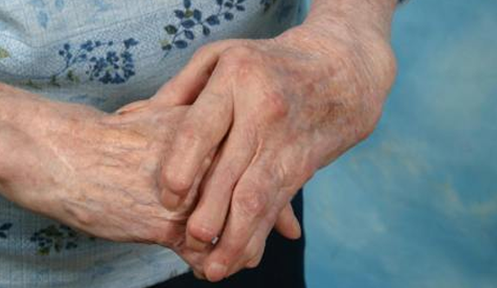
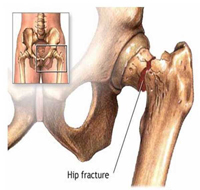 There are a number of conditions, which can result in a patient having to undergo hip replacement surgery. Perhaps the most common condition is osteoarthritis that is commonly referred to as 'wear and tear arthritis'. Osteoarthritis can occur with no previous history of injury to the hip joint. The hip simply 'wears out'. There may be a genetic tendency in some people that increases their chances of developing osteoarthritis.
There are a number of conditions, which can result in a patient having to undergo hip replacement surgery. Perhaps the most common condition is osteoarthritis that is commonly referred to as 'wear and tear arthritis'. Osteoarthritis can occur with no previous history of injury to the hip joint. The hip simply 'wears out'. There may be a genetic tendency in some people that increases their chances of developing osteoarthritis.Avascular necrosis is another condition that could lead to hip replacement surgery. In this condition, the femoral head (ball) loses a portion of its blood supply and actually dies. This leads to collapse of the femoral head and degeneration of the hip joint. Avascular necrosis has been linked to alcoholism, fractures and dislocations of the hip and long-term cortisone treatment for other diseases.
Abnormalities of hip joint function, resulting from trauma to the hip, fracture of the hip, and some types of hip conditions that appear in childhood, such as congenital dysplasia of the hip (CDH) can lead to degeneration many years later. The mechanical abnormality leads to excessive wear and tear.
-
Types of Implants
+ Each section has an ODEP rating listed. This is a rating issued by a group of medical professionals. The number refers to the minimum number of years that the implant has been around (3 being a low number of years and 10 being the highest) and the letter refers to the quality of published data that supports the implant (a. being the best c. being the worst). So far, this regulatory body has rated only hips.
Each section has an ODEP rating listed. This is a rating issued by a group of medical professionals. The number refers to the minimum number of years that the implant has been around (3 being a low number of years and 10 being the highest) and the letter refers to the quality of published data that supports the implant (a. being the best c. being the worst). So far, this regulatory body has rated only hips.Types of Hip Replacement 

Re-surfacing Un-cemented 

Cemented Revision Resurfacing Hip
Fixation
Fixation of the cup in hip resurfacing is with a press-fit fixation initially. The surface of the cup on the outside is such that bone will grow into it to anchor it in place. The fixation on the femoral side is with cement. The resurfacing does not rely on a stem to go into the femoral canal around which the cement can get a grip. The femoral resurfacing chamfers the femoral ball and is then cemented over the top of this chamfered bone. This means on the femoral side that only a minimal amount of bone is removed. It does however mean that the bone within the femoral neck is relied upon to give support. Particularly in women, the quality of this bone becomes poor as the patient gets older with an increased risk of osteoporosis. For this reason, a resurfacing tends to be done more frequently in men and of a younger age group.
The bearing surface
The bearing surface is a metal on metal bearing surface. Because of the design of the component the metal head accurately reflects the true size of the femoral head and this gives a very natural feeling hip. The bearing surface is described as metal on metal but in fact will have a film of fluid between the two metal surfaces.
Stability
The large metal head gives the resurfacing excellent stability.
Durability
The long-term results of hip resurfacing are not yet known. Over the years, hip resurfacing has failed, primarily because of manufacturing problems. The newer manufacturing techniques have allowed a much better resurfacing to be made and with this, it is expected that the results will be better. Over the next few years, 10-year results will become available on the modern resurfacings.
Extra large heads
The benefit of the resurfacing described above appears to be the bearing surface with a femoral head, which is of normal anatomical size. This appears to give a natural feeling hip. The big disadvantage is that it can only be used on patients with good quality bone. The other disadvantage is that access to the hip is difficult because the head is retained. This means it is difficult to do the operation through a small incision. An increasingly popular joint replacement is now to combine the resurfacing head with a femoral stem.
The head is placed onto the stem with a Morse taper to allow the benefits of the resurfacing technology to be put onto a more conventional stem.
Un-cemented Hip
Cementless Stem
The stem is implanted into your femur (thighbone). These rely on a tight fit initially to give "press-fit" stability but in the longer term rely on bone growing into or onto the prosthesis to hold it in place. Both cemented and cementless systems can be very successful and your surgeon will choose whichever system he is most comfortable with using.
Cementless Cup
The cup is implanted into your acetabulum (socket). These also rely on a tight fit initially. Cementless cups are made up of two parts. The shell is made of metal and an insert that site inside of the shell. Inserts can be made from plastic, ceramic or metal. Your surgeon will decide which is best for you depending your activity and lifestyle.
Cemented Hip
In the 1960's Sir John Charnley who worked at Wrightington Hospital, Wigan, produced a total hip replacement. Prior to this attempts had been made to replace the hip using ceramic or glass femoral heads but it was Sir John Charnley, both an engineer and surgeon, who designed and used hip replacements that have, with the passage of generations, become the most popular today. Cemented hip replacements have a cup that fits into a pelvic socket or acetabulum and will also have a femoral stem that fits into the femoral shaft and on the top of this stem will be a ball that articulates with the acetabular component.
Initially in England, the emphasis was on using cement as this was the way the Charnley hip was made. Another popular hip is the Exeter hip. This is again uses cemented; the cement is used to fill the gap between the implant and the bone. The cement does not work as an adhesive but as filler.
Cementless Stems
A revision hip is used when previous hip surgery has failed or worn out. Revision hip stems can be either cemented or cementless and are always made of metal. Usually revision hip stems are bigger than primary hip stems to accommodate any bone loss. Usually the surgeon will need to be stem fixation in other areas of the thigh bone (femur) than obtained during the first procedure, therefore there are many different revision hips stems to accommodate these needs, for example, often bone further down the femur (towards the knee) provides better fixation points, therefore longer hip stems are often used.
A revision cup is usually uncemented, however, cemented cups are often used in revision, with bone defect being filled with artificial bone.
-
Investigation
+If you are advised hip replacement surgery you may require to undergo:
- Evaluation of status of your teeth, ear, nose, throat and kidneys to rule out hidden infection.
- X-ray of your chest.
- ECG, 2D echo.
- Investigations as follows:
 CBC, ESR, Blood sugar fasting and after lunch
CBC, ESR, Blood sugar fasting and after lunch Blood group and Rh factor
Blood group and Rh factor Kidney function tests, Liver function tests
Kidney function tests, Liver function tests Test for HIV
Test for HIV Test for Australia Antigen
Test for Australia Antigen Test to rule out Hepatitis C
Test to rule out Hepatitis C Routine examination of your stool and urine
Routine examination of your stool and urine Special tests if indicated
Special tests if indicatedAfter assessing your reports, you will be referred to a physician for medical fitness, and to the anaesthetist for evaluation.
Prior to surgery, you will be familiarised with the exercises, which you will be required to do after the surgery.
-
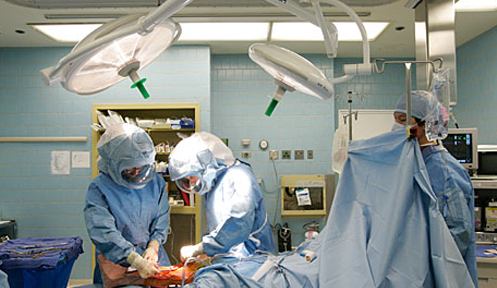
Operations
+If the surgery is scheduled for the morning, be ready after brushing your teeth. You will be taken to the operation theatre at the time, which will be informed the previous night.
If your surgery is scheduled for afternoon, you may be allowed tea/coffee and light breakfast early morning of the operation day.
Some medicines may be required to be taken by mouth on the morning of surgery with few sips of water and some injections may be administered prior to being taken to the operation theatre.
At the appointed time, you will be taken to the operation theatre.
While being taken to the operation theatre, please remember:
- To remove contact lenses.
- To remove spectacles.
- To remove jewellery.
- Not to carry cash or valuables.
In the operation theatre, the anesthetist would connect you to various monitors and check-up your heart, oxygen saturation and blood pressure. Before starting the anesthesia, an intravenous line in the forearm will be taken to administer various medications.
As discussed previously you will be administered the anesthesia most suitable for you. If it is going to be Epidural anesthesia, you will be made to sit and your lower back will the cleansed with an antiseptic solution. Then after numbing your skin, a thin tube will be inserted in your back with the help of a special needle.
Once you are anaesthetised, a catheter may be put to ease passing urine.
The actual preparation for the operation consists of thorough cleansing of the leg and covering it with sterile drapes.
-
Post Operative Treatment
+Your Hospital Stay:
You should be admitted to hospital in good time before your operation to allow time for you to settle in. Your anesthetist will examine you by checking your heart and chest. This is an opportunity for you to ask any questions before your operation.
On the day of your operation, it is usual that your doctor will ask you not to drink or eat anything. The area around your hip may be shaved to reduce the risk of infection.
An hour or before the operation you will be given medicine to relax you. This is known as a "pre-med". You will then be taken into the operating theatre where you will be given your anesthetic and have your operation.
The operation usually takes 1-2 hours to complete.
 Immediately after your operation, you will be moved to the recovery room for close monitoring. You will have one or two drips in your arm to put fluid back into your body. When you wake up from surgery, your leg may be swollen and bruised and the muscles may be stiff and sore. Your new joint should not cause you any discomfort, but you may experience some pain from the surgical procedure itself. You will be given pain medications to take regularly whilst you are recovering.
Immediately after your operation, you will be moved to the recovery room for close monitoring. You will have one or two drips in your arm to put fluid back into your body. When you wake up from surgery, your leg may be swollen and bruised and the muscles may be stiff and sore. Your new joint should not cause you any discomfort, but you may experience some pain from the surgical procedure itself. You will be given pain medications to take regularly whilst you are recovering.When you are fully conscious, breathing well and your blood pressure and pulse are stable, you will be taken back to ward. You probably will not feel much like eating at first, but it is important that you drink. The scar on the side of the hip should eventually fade to a thin white line.
 During the next few days, the drips will be removed. Your physiotherapist web visit you the day after your operation to commence you on your exercise programmed and help you get back on your feet walking again. You may feel unstable and in pain at first, but you will be given a frame to help you walk with, then crutches or sticks, which you may need for four to six weeks after, depending on your surgeon's instructions.
During the next few days, the drips will be removed. Your physiotherapist web visit you the day after your operation to commence you on your exercise programmed and help you get back on your feet walking again. You may feel unstable and in pain at first, but you will be given a frame to help you walk with, then crutches or sticks, which you may need for four to six weeks after, depending on your surgeon's instructions.Once you, your surgeon and physiotherapist are happy with your condition and mobility you will be discharged from hospital. The usual hospital stay for hip joint replacement is usually four to seven days.
-
Complications
+In the long term, many problems relate to osteolysis from acrylic bone cement debris, and/or wear debris. An inflammatory process causes bone resorption and subsequent loosening or fracture often-requiring revision surgery. Very hard ceramic bearing surfaces are being used in the hope that they will have less wear and less osteolysis with better long-term results. Large metal heads (metal-on-metal hip arthroplasty) are also used for similar reasons as these also have excellent wear characteristics and benefit from a different mode of lubrication.
 However, large fixed metal heads, such as the Austin Moore devices, can result in protrusio acetabuli. A greater head neck ratio also contributes to stability. These new prostheses do not always have the long-term record of accomplishment of established metal on poly bearings. As metal-on-metal arthroplasty becomes more widespread, concerns are being raised about the potential dangers of metal particulate debris. There are new publications that have demonstrated development of pseudotumors, soft tissue masses containing necrotic tissue, around the hip joint. It appears these masses are more common in women and these patients show a higher level of iron in the blood. The cause is unknown and is probably multifactorial. There may be a toxic reaction to an excess of particulate metal wear debris or a hypersensitivity reaction to a normal amount of metal debris.
However, large fixed metal heads, such as the Austin Moore devices, can result in protrusio acetabuli. A greater head neck ratio also contributes to stability. These new prostheses do not always have the long-term record of accomplishment of established metal on poly bearings. As metal-on-metal arthroplasty becomes more widespread, concerns are being raised about the potential dangers of metal particulate debris. There are new publications that have demonstrated development of pseudotumors, soft tissue masses containing necrotic tissue, around the hip joint. It appears these masses are more common in women and these patients show a higher level of iron in the blood. The cause is unknown and is probably multifactorial. There may be a toxic reaction to an excess of particulate metal wear debris or a hypersensitivity reaction to a normal amount of metal debris.Postoperative sciatic nerve palsy is another possible complication.
A few patients who have had a hip replacement suffer chronic pain after the surgery despite normal imaging.
-
FAQ
+If you are advised Hip Replacement surgery, you may want to know more details about it. Here we list the most commonly asked questions about hip replacement and their answers. If you want any further clarification, please do not hesitate to ask either Dr. Rakesh Rajput or one of his associates.
Q. What are the conditions, for which the hip replacement is advised?
A. Hip replacement is advised for many painful hip disorders like fresh or old fractures of either the socket or the ball, failure of previous fixation and arthritis of the hip.
Q. For which painful hip disorder, hip replacement can not be done?
A. If the hip pain is due to ongoing infection in the joint or the bones, hip replacement is contra indicated. However, if the infection is burnt out, one may carry out hip replacement is selected case
Q. At what age can joint replacement be done?
A. Joint replacement is ideally done for patient above the age of 60 years. It may be done between ages of 40 and 60. It is rarely done between ages of 20 and 40. It is never done in children. Currently the qualities of the artificial joints being very good, young people, even in their 20s & 30s, who suffer from painful arthritis, are advised to undergo early surgery to improve the quality of life.
Q. What are the types of hip replacements?
A. There are three types of hip replacements; Hemi replacement : In which only ball of the femur is replaced. Total hip replacement: In which ball is replaced and the socket is resurfaced. Surface replacement: Where the surface of the ball is shaved off and is capped and similarly the surface of the socket is scraped off and is resurfaced with metal lining. Hemi and total replacement may be either cemented or Non-cemented.
Q. What is the difference between cemented and non-cemented hips?
A. The parts of the artificial hip may either be fixed to bone with a substance called Methyl Methacrylate (Bone cement), or they are press fitted to the bone with capacity for the bone to stick to the parts. This Non-cemented hip is used mainly for younger individuals.
Q. What is the ball and socket made up of?
A. The ball is made of either stainless steel or cobalt chrome alloy or ceramic. The socket is made of either polyethylene or stainless steel or ceramic.
Q. What is the average time taken for surgery?
A. The average time taken for joint replacement surgery is 1 hour and 30 minutes.
Q. What is the average hospital stay recommended after joint replacement?
A. The hospital stay is approximately for seven days after hip replacement surgery.
Q. When does the exercise program start after joint replacement?
A. Exercises start within a day after joint replacement, while walking starts 2 - 3 days after the surgery
Q. Does one need some support of walker or stick after joint replacement?
A. One may need temporary support of walker or walking stick after joint replacement. Whether one needs permanent, support depends on whether other joints are affected.
Q. Can a person with diabetes, high blood pressure, heart trouble undergo joint replacement?
A. Even a person with diabetes, high blood pressure, heart trouble can safely undergo joint replacement surgery under medical supervision.
Q. What are the precautions to be taken after joint replacement?
A. It is advisable to use commode, avoid sitting on floor, jogging, running and fast sports after joint replacement surgery. Moderate speed walking, climbing stairs and swimming are permitted.
Q. What are the common complications after joint replacement?
A. The complications after joint replacement are Deep vein thrombosis, pulmonary embolism and Infection.
Q. What precautions are taken to prevent these complications?
A. To prevent deep vein thrombosis, at our centre we use calf compression device, which gently massages the calf, preventing blood flow stagnation. In some patients, blood thinners are administered. To prevent infection, surgery is carried out in specialised operation theatre at our centre; we use space suits during surgery to prevent wound contamination and use antibiotics pre-operatively. With our system of Navigation with computer, the chances of fat embolism have reduced considerably.
Q. Can this operation be done in any Nursing Home or Hospital?
A. No, this is a specialized surgery, which requires a special set up. This includes proper operation theatre, post-operative intensive care unit, trained nurses and technicians along with expert physiotherapist to achieve desired results.
Q. How much does the surgery cost?
A. The cost depends on the type of Implant, the type of room that you select and your medical condition. Before surgery, a budget can be drawn out.
Q. Is it covered under Mediclaim?
A. That will depend on the Mediclaim policy.

Dr. Rakesh Rajput
MBBS (Cal), MS Orth (Cal), FRCS (Glasgow)
MCh Orth (UK), FRCS Trauma & Orth (UK)
Director and HOD, Dept. of Orthopedics CMRI Hospital, Kolkata President AOPAS Specialist in Total Knee Replacement, Hip Replacement, Joint Replacement, Arthritis, Arthroscopy, Pelvic & Acetabular Trauma |